
Blastocyst Culture and Transfer in Ahmedabad
- Have you experienced multiple IVF cycle failure?
- Do you want to minimize the risk of multiple pregnancies in IVF?
If yes, then we at Nisha IVF Centre can address these problems through Blastocyst Culture and Transfer in Ahmedabad.
Blastocyst culture is the method of developing embryos in an IVF laboratory till they reach the blastocyst stage. Then, transferring the resulting embryo in the woman’s uterus.
Visit us at Nisha IVF Centre, one of the top IVF Centres in Ahmedabad. We have obtained a higher success rate of IVF procedure during the first cycle for most patients.
At Nisha IVF Centre, we specialize in a wide range of advanced reproductive treatments, including IVF, ICSI, IUI, Cryopreservation, Frozen Embryo Transfer, etc. Our IVF doctors in Ahmedabad provide the most effective and cost-efficient treatments to our patients to achieve a successful pregnancy.
What is a Blastocyst?

- Blastocysts have a large, central, fluid-filled cavity and two distinct cell types. A blastocyst is a preimplantation embryo that can be considered the last stage of embryonic development outside the body.
- After the egg retrieval process, in the IVF laboratory, fertilization is carried out by IVF or by ICSI procedure. The embryologist places the resulting embryos in an incubator for further growth.
The stages of embryo development are as follows:
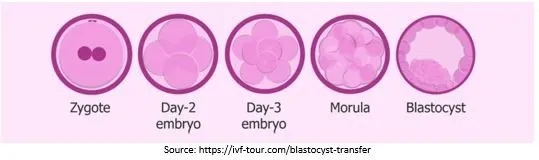
- The day of egg retrieval is counted as day 0
- The pronuclear stage on day 1 (embryologist examines how many eggs have successfully fertilized)
- The two to the four-cell stage on day 2
- The eight-cell stage on day 3
- The morula stage on day 4
- The blastocyst stage on day five or day 6
After this stage, the embryo needs the uterus for blastocyst implantation and further development. The blastocyst has two distinct cells, unlike only one cell type in early cleavage stage embryos.
Different Cell Types of a Blastocyst are:

- Inner cell mass
The cells in the centre of the blastocyst are called the inner cell mass. After implantation, the inner cell mass gets converted into the foetus.
- Trophectoderm
The single-cell layer outside the blastocyst forms the trophectoderm that gradually gives rise to the placenta.
- Previously, almost all IVF centres used to transfer embryos at the cleaving pre-embryo stage (usually 4-16 cells). It required culture of the embryos for two to three days in the laboratory.
- The recent development of advanced sequential culture media has allowed embryos to be cultured for 5-6 days to reach the blastocyst stage.
Who can benefit from Blastocyst Culture?
The fertility experts suggest Blastocyst culture for:
- Patients with multiple failed IVF cycle:
Executing a blastocyst culture on a patient with failed IVF with day 2/3 embryo transfer can yield more information about the embryos’ growth and improve the pregnancy rate.
- Eliminating the risk of multiple pregnancies:
Blastocyst culture allows the transfer of the single and high-quality embryo, decreasing the chance of multiple pregnancies.
Looking for an IVF Treatment?
Fill Out the Form Below for an instant Appointment with the Doctor
What are the advantages of blastocyst culture?
- Extended embryo culture in IVF probably enables the identification of embryos with higher developmental ability.
- It also benefits in synchronizing embryonic age with endometrium to promote early communication between the two.
- This technique includes more than a single culture medium to supply the metabolic requirements of the developing embryo.
- The rate of blastocyst formation per fertilized oocyte is 30-40 % at present.
Other benefits include –
- More physiological
- High implantation rate
- Gives us a chance for a better embryo selection
- Increases the predictive value of pregnancy
- Decreases multiple pregnancy rates as a smaller number of embryos are transferred.
- More suitable for PGD and Cryopreservation
Are there any drawbacks of blastocyst transfer?
- It applies to a group of selected patients of younger age and those with moderate to good response to the stimulation protocols.
- Higher embryo transfer cancellation rate because of no blastocyst situation
- More risk of monozygotic twin birth
- More embryo wastage as lesser embryos reach the blastocyst stage in vitro
- Few groups reported similar pregnancy rates with Day two and Day three embryo transfers. It leads to prolonged in vitro culture of embryos and increases laboratory expenses.
Blastocyst culture is a promising method. But it must be correctly used in the existing IVF setup. An unexpected changeover to the day five transfer may not meet the expectations. Like, its use should be decided on a patient-to-patient ICSI basis and not be generalized to all, to avoid disappointments.
If you are trying to conceive for longer, we suggest you consult our fertility experts at Nisha IVF Centre. You can book an appointment or contact us at +919081233800, +912717233800.
Frequently Asked Questions
Can one walk after the embryo transfer?
An embryo must attach to the uterine wall at this time before it can fully implant, which may take a few days. Hence, for the first one to two days, stay home, and take rest. Avoid strenuous activities such as heavy lifting, bending, or exercise.
How long does a blastocyst take to implant?
In IVF, the fertilized eggs or human blastocysts usually hatch out of their shell and implant about 1 or 2 days after the fifth day of the blastocyst transfer. It means the implantation occurs about 7 to 8 days after fertilization of the egg.
What happens if an IVF transfer fails?
After a failed IVF, it’s vital to grieving. Even if the IVF didn’t result in an embryo, the emotional impact is as devastating as the loss of a pregnancy. You’ll feel gloomy and depressed for a long time. It’s quite normal, but you should consult your doctor about it.
